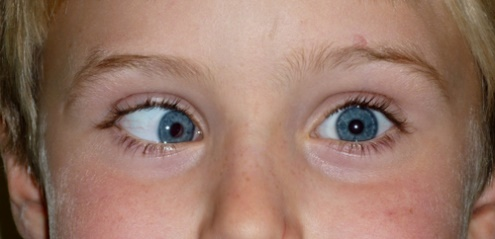
Binocular Vision
Binocular vision, or binocularity, means the ability to use the two eyes as a pair. They are co-ordinated and obey certain physical laws of innervation. Binocular vision is the basis for stereopsis, or 3D vision, and straight eyes are essential for its development.
Glasses
Glasses are prescribed to children after they are tested for refractive errors, which is the need for glasses. In children, eye-drops, usually cyclopentolate, are used prior to a refraction to dilate the pupils and the test is carried out. There are different types of refractive errors. See below:
Hyperopia (Hypermetropia, Farsightedness, Or Longsightedness)Hyperopia is a refractive error of the eye, causing a difficulty in near focussing, although in high amounts, it affects all distances. It is usually caused by the eyeball being too short in length, or by the cornea in the front of the eye being too flat. This results in an inability to focus light rays sharply on the retina, which causes blurred vision.
This condition is present at birth, and tends to improve with time as the eye grows. In fact, it is normal to be born with a low amount of hyperopia. Moderate to large amounts of hyperopia in children can cause accommodative esotropia and amblyopia.
Hyperopia is sometimes confused with presbyopia, see below.
Myopia (Shortsightedness, Nearsightedness)Myopia is an optical anomaly within the eye, causing distance vision to be blurred, and near vision to be clear. There can be different causes, but it is usually caused by the eyeball being too long, or the cornea at the front of the eye being too curved.
Myopia can be present at birth, but this is uncommon. It is more usual to develop later in childhood, or during the early teens, and tends to worsen as the eye grows.
AstigmatismAstigmatism is a common optical defect of the eye, where there is a difference in the degrees of refraction in different meridians of the eye. This causes vision to be blurred or distorted at all distances, as the eye is incapable of focussing an image sharply. It is usually caused by the cornea, or the front part of the eye, being an irregular shape. A common analogy used is the description of the eye being shaped like a rugby ball instead of a (spherical) football.
Astigmatism can be corrected with glasses, using a lens that has different radii of curvature in different planes, known as a cylindrical lens. It can also be corrected with contact lenses or refractive surgery.
PresbyopiaPresbyopia is the term used to describe the inability of the eyes to focus on near objects as a person ages, giving rise to the need for reading glasses. The usual age of onset is between 40 and 50 years.
Glasses And ChildrenWe are often asked how it can be possible to know if a child, or even a baby, needs glasses.
For this, a refraction, or retinscopy , is carried out, usually by an ophthalmologist, after dilating the pupils. Dilating the pupils is necessary because the examiner must observe the movement of a light on the red reflex on the retina, using a retinoscope.
This process objectively measures the refractive error of the eye. It can usually be done quickly, accurately and with miminal co-operation from the child.
If there is a significant refractive error, glasses are recommended, or the child may be closely monitored at regular appointments until it becomes apparent that they would benefit from glasses. At these appointments, the orthoptist will assess vision and make sure the eyes are working together. If there is any sign of amblyopia, or a squint, a prescription for glasses may be recommended.
Usually it is recommended that the glasses are worn full-time. As the eyes are growing throughout childhood, it is often difficult to say initially for how long the glasses will need to worn.
Parents are often concerned that the child won’t want to wear the glasses, that they may be teased at school, or that the child may be restricted in playing sport. We find that this is now rarely a problem, because of several factors. There is a great choice of children’s glasses available, and it can be a good idea for the child to be encouraged to choose their own pair, e.g., a favourite colour or cartoon character. Harry Potter has been a great advocate for children’s glasses! As well as this, as services have improved, we have become much better at picking up problems earlier, and therefore, it is not unusual to see young children wearing glasses. This has made it much more socially acceptable.






Wearing glasses for sport can be a problem in older children, when sport becomes more physical. However, there are now sports glasses available, which can be worn for football, rugby, GAA.
Strabismus (squint)
Strabismus is the correct term for any misalignment of the eyes. It is often called a squint, a crossed eye, or a turn in the eye. There are many different types. Strabismus is usually categorised according to the direction of the turn. An inward (converging) turn is called an esotropia. An outward (diverging) turning eye is called an exotropia. Vertical strabismus occurs when the eye turns downwards, called a hypotropia, or upwards, called a hypertropia. It is also possible but much less common for the eye to be twisted out or in. This is known as a cyclotropia. Strabismus can occur in childhood or adulthood, depending on the cause.